Hypospadias
Hypospadias is an anomaly in the formation of the penis during gestation that manifests itself, fundamentally, in three ways:
- The opening where urine comes out (called the meatus) is often narrow and not at the tip of the penis.
- The penis presents a ventral downward incurvation, more evident in erect position.
- There is a ventral preputial skin defect and dorsal cutaneous excess.
Hypospadias are classified as follows:
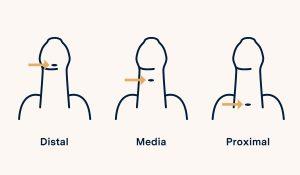
- Distal: these are the most frequent. It occurs when the meatus is close to the glans penis and the incurvation and skin defect are milder.
- Medium: those in which the malformation is more severe.
- Proximal: those in which the meatus is located at the base of the penis or even in the scrotum.
In a significant percentage of cases, especially in the most severe hypospadias, it may be associated with other anomalies, the most frequent:
- Peno-scrotal transposition is an anomaly of the external genitalia in which the scrotal skin arises above the penis.
- Uni-bilateral cryptorchidism is the absence of one or both testicles in the scrotal pouch.
- Prostatic utricle: is an anomaly in the formation of the internal genitalia that occurs frequently in children with severe hypospadias. It consists in the permanence of an embryonic remnant resulting from the formation of the internal genitalia during pregnancy and resulting in a "cul-de-sac" in the posterior urethra. It may become evident in episodes of urinary tract infection, lithiasis or difficulty in catheterization in these patients.
Symptoms and causes of hypospadias
The causes of hypospadias are considered to be multifactorial, that is, genetic factors and multiple environmental factors are involved.
Regarding the symptoms, the presence of hypospadias is suspected in the presence of a pressurized urinary stream directed downward, the presence of ventral incurvation in the erection and excess skin in the dorsal area.
The child's glans penis is usually covered by the balanopreputial adhesions, so it is common that the actual position of the urinary meatus cannot be appreciated with certainty.
Diagnosis of hypospadias
Assessment by a pediatric urologist is important to identify mild cases, reassure parents, rule out other abnormalities if necessary, and schedule intervention at an appropriate age.
The diagnosis is made by means of a thorough inspection in consultation, in which the patient is assessed:
- The position and size of the meatus.
- The presence or not of penile incurvation.
- The quality and disposition of the preputial skin.
- The numerous anomalies often associated with this pathology: webbed penis, peno-scrotal transposition, bifid scrotum, cryptorchidism...).
In severe hypospadias, urological ultrasound may be necessary to rule out other associated pathologies.
Hypospadias treatment
Hypospadias can be treated by surgery and must be performed by a pediatric urologist specialized in the management of this pathology.
Hypospadias is usually treated from the age of one year of life onwards, but the optimal age for this intervention can be individualized according to the severity of the malformation and personal circumstances.
The objective of this treatment is to correct the incurvation, to bring the orifice to the glans and to achieve a good aesthetic result. To carry it out, different techniques can be used, which will vary depending on the characteristics of the disease and the patient, but the final assessment, the choice of the best technique in each case and the planning in one or two interventions, will be made in one or two interventions. The definitive evaluation, the choice of the best technique in each case and the planning in one or two interventions, is often considered on the same day of the intervention.
The surgery usually lasts between one or two hours depending on the technique used. During the immediate postoperative period, the patient has a bladder catheter to avoid complications and a dressing around the penis that will not be removed until the seventh postoperative day. After the removal of the catheter, the patient recovers the usual continence and it is not necessary to remove the stitches, since they fall out by themselves with the passing of the days.
After the intervention and the removal of the catheter, the patient must attend check-ups in the office to evaluate the aesthetic result, the presence and characteristics of the erections and the urinary stream.

Complications and prognosis
The most frequently described complication in the literature is the appearance of a urethral fistula, which is a small hole in the path of the operated area, through which urine leaks out.
To avoid this complication, all necessary measures are taken to take meticulous care of the tissues and protection of the sutures by means of vascularized flaps, thus reducing the possibility of this complication occurring.
The follow-up of these patients continues after the intervention, although each time in more spaced visits, until the child's growth is complete. In this way, the pediatric urologist can assess the long-term outcome and ensure that the patient's questions and concerns are resolved.
Team of the Hypospadias unit


 +34 912 627 104
+34 912 627 104 Contact
Contact







