Miniperc Percutaneous Nephrolithotomy
The risk of bleeding, possible complications and hospitalization time is lower than with other percutaneous nephrolithotomy techniques.

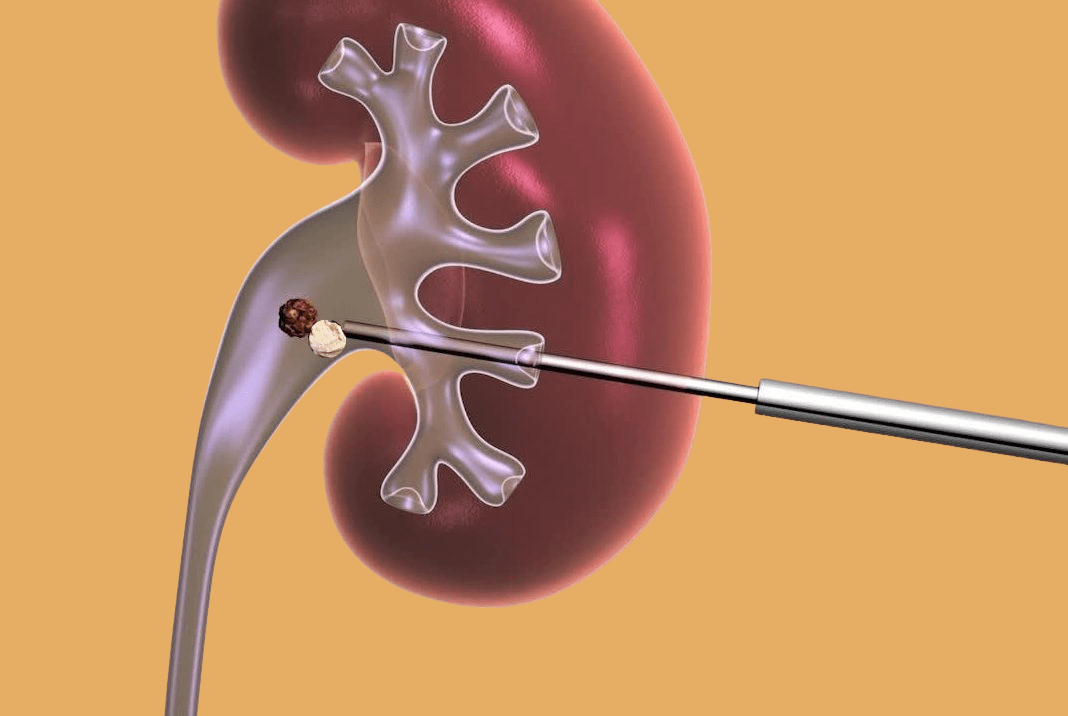
What is Percutaneous Nephrolithotomy with Miniperc?
Percutaneous mini-nephrolithotomy, also called mini-PNL or Miniperc, is an effective and safe technique for the treatment of small and medium-sized kidney stones. Stones of 10 to 25 mm may be ideal candidates for miniaturized PNL.
It is a procedure similar to percutaneous nephrolithotomy (removal of kidney stones through the skin) with the difference that the skin incision is smaller - hence the name miniperc - and therefore the risk of bleeding is reduced, the complications inherent to dilatation are also reduced and the hospitalization time is shorter.
Percutaneous nephrolithotomy (PNL) is considered the standard treatment for kidney stones larger than 2 cm, but it can also be considered a valid option for stones between 1 and 2 cm in size, as recommended by the European Guidelines on Lithiasis.
Since the first percutaneous nephrolithotomy was performed in 1976 by Fernstrom and Johansson, this technique has undergone important changes in different aspects that have increased its efficacy and safety: different ways of positioning the patient have been described, new fragmentation energies have emerged, as well as different ways of dilating the tract.
The learning obtained along this journey and the limitations that have been detected in other renal lithofragmentation techniques, such as retrograde surgery or extracorporeal shock wave lithotripsy, have led the international urological community to accept miniaturization as the main trend in percutaneous nephrolithotomy (PNL) in the last 15 years.
In addition to reducing the diameter of the external tract and the working instrument (nephroscope), miniperc involves other modifications in the lithotripsy technique for the benefit of the patient's postoperative comfort. Among these modifications are the use of laser technology for stone fragmentation or pulverization, the reduction of the extraction elements, the reduction of the nephrostomy caliber (opening from the outside of the body to the renal pelvis) and a different exit strategy.
Laser systems using high-power, high-frequency thulium or holmium fibers can further optimize results.
However, the miniperc technique also has some limitations, such as longer operative time due to the reduced caliber of the percutaneous tract, potentially higher intrarenal pressure, complications such as postoperative fever or sepsis due to increased pyelotubular reflux, or a greater number of residual fragments.
Faced with this paradigm shift in percutaneous nephrolithotomy, it is necessary to have highly experienced surgeons who are accustomed to this new concept in the percutaneous approach to lithiasis.
- Ideally indicated in stones from 10 to 25 mm of any composition and renal or proximal ureteral location.
- More extensive stone disintegration is required due to smaller tracts and limited ballistic lithotripsy systems compared to conventional PNL.
- The use of laser as a lithofragmentation tool further improves efficiency and outcome.
- Lower complication rate with less bleeding and shorter hospitalization time.
- The greater the miniaturization, the greater the intrarenal pressure.
- It can lead to an increase in residual fragments because the extraction elements are not efficient, requiring, on some occasions, a second time with different approaches to solve the problem definitively.
| NLP standard ( 24F) | NLP miniaturizada (<18F) | |
|---|---|---|
| Lithiasis size | > 20-25mm | 10-25mm |
| Composition | Any | Any |
| Location | Renal and/or proximal ureteral | Renal and/or proximal ureteral |
| Fragmentation | Ballistic-Ultrasonics TRILOGY | Laser |
| Bleeding | Mayor | Menor |
| Intrarenal pressure | Menor | Larger as caliber decreases |
| Hospitalization time | Mayor | Menor |
In the Lithiasis Unit of ROC Clinic we have miniaturized nephroscopes of different calibers and renal access sheaths that allow us to perform these techniques satisfactorily. On the other hand, our wide and extensive experience in the use of Holmium and Tulium laser enables us to perform very efficient fragmentations. This is reflected in our results, with a lithiasis-free rate of more than 90%.
+100
Miniaturization has been the main trend in percutaneous nephrolithotomy (PNL) in the last 15 years.
Newsof ROC Clinic in Percutaneous Nephrolithotomy Miniperc
Research
Minimally Invasive Techniques for Large-Volume Benign Prostatic Hyperplasia: A Comparative Study of HoLEP and Robotic Simple Prostatectomy
They ask us in the Consultation
See more questionsTeam of the Miniperc Percutaneous Nephrolithotomy Unit.
No professionals were found.


 +34 912 627 104
+34 912 627 104 Contact
Contact





