Treatment Bladder cancer
Pioneering technology for the treatment of bladder cancer.
Survival rates for bladder cancer are high, but it is also a highly recurrent cancer, making it one of the most expensive cancers to treat and monitor.
- Super-specialized urologists
- Personalized treatment
- Minimally invasive approach
- More than 16,000 patients successfully treated
Bladder cancer treatments
Once bladder cancer has been diagnosed, different treatment options will be employed depending on the characteristics of the tumor, the stage of the disease and other factors such as the patient's age or general health.
Treatments for non-musculoinvasive bladder cancer
Transurethral bladder resection
When the tumor is at an early or superficial stage, it can be treated with a transurethral resection of the bladder (TUR). This surgical procedure is used for both diagnosis of bladder cancer and treatment of the tumor.
To perform this procedure, a transurethral resector is introduced into the bladder through the urethra (endoscopic procedure). Once inside, a visual examination is performed to identify all tumorous or suspicious lesions (cystoscopy). Subsequently, the tumor tissue is removed (resection) using electrical energy that heats the resector, reaching the optimal temperature to cut and cauterize the affected tissue.
This procedure also makes it possible to obtain a tumor sample for anatomopathological diagnosis and subsequent staging.
This treatment usually requires spinal anesthesia (local anesthesia injected into the back), although it may vary according to the needs of the patient and the anesthesiologist who applies it. The patient must also be given prophylactic antibiotics to reduce the risk of infection.
This technique ends with the placement of a bladder catheter with a continuous saline flushing system to prevent clot formation.
The duration of this surgery can vary from 30 to 90 minutes depending on the number, size or location of the tumors. Hospitalization time can last from 1 to 2 days.
Intravesical chemotherapy
Chemotherapy is the use of certain drugs to prevent cancer cells from growing or to cause their death.
In intravesical chemotherapy, the drugs are administered directly into the bladder through a catheter inserted into the urethra. It is a local treatment and therefore only destroys superficial tumor cells that come into contact with the chemotherapy solution. It does not reach tumor cells infiltrating the bladder muscle or those that have spread to other organs. For this reason, intravesical chemotherapy is only used for non-muscle invasive bladder cancers. The drugs most commonly used in intravesical chemotherapy are mitomycin-C, gemcitabine and thiotepa . Other drugs used include cisplatin, doxorubicin and valrubicin (Valstar).
Intravesical chemotherapy is administered with different treatment schedules starting a few weeks after bladder TUR to reduce the likelihood of tumor relapse. There is also the option of administering a postoperative dose of mitomycin C in the first 24 hours after TUR, with the aim of eliminating those tumor cells that may have remained "floating" in the bladder after the operation and thus avoiding their implantation in the walls, giving rise to a relapse of the tumor.
The nurse inflates the urinary catheter bulb with leg drainage bag in the sterile field.
Intravesical immunotherapy
Immunotherapy is the use of drugs that help the immune system recognize and destroy cancer cells and prevent cancer from reproducing and progressing.
Occasionally, after transurethral resection of the bladder, immunotherapy with bacillus Calmette-Guérin (BCG), an attenuated bacterium that can help provoke an immune response when bladder cancer is not infiltrative, can be administered. It is administered directly into the bladder by bladder catheter or catheter in order to prevent tumor recurrence or progression of previous tumors to more advanced stages.
To determine whether the patient requires these therapies, several factors are taken into account: local stage, tumor grade, size of the lesions removed, history of previous recurrences or presence of associated carcinoma in situ, as well as the patient's general condition and an evaluation of the patient's other pathologies.
Typically, BCG instillations are performed once a week for six weeks in the induction period and then several boosters are performed in three-week batches with varying frequency for a minimum of one year and a maximum of three years (maintenance period).
Treatments for musculoinvasive bladder cancer
Radical cystectomy and reconstructive surgery
First, a bladder TUR will be performed to establish the diagnosis of tumor infiltration of the muscular layer. Once the diagnosis is made, a radical cystectomy (removal of the bladder) can be performed with curative intent. Cystectomy in men includes removal of the bladder, prostate and seminal vesicles. In women, it involves removing the bladder, uterus, ovaries, cervix and part of the vagina. The pelvic lymph nodes must also be removed in both sexes.
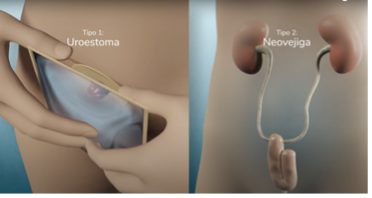
In the same surgery, the surgeon must create a urinary diversion, i.e. a new way of storing urine and allowing it to be eliminated from the body. For this purpose, there are different techniques that the physician must evaluate. Among the most commonly used are the neobladder, which consists of creating a new bladder from the intestine; cutaneous ureterostomy, which consists of ablating the ureters to the skin of the abdomen; and cutaneous ureteroileostomy, which consists of anastomosing (joining) the ureters to a portion of intestine that will allow urine to exit through the stoma made in the patient's skin. This surgery can be performed through an open approach; laparoscopic, that is, by means of a camera that transmits the magnified image to a monitor, allowing the surgeon to intervene inside the patient without making large incisions; or robotic, which allows complex procedures to be performed in a less invasive manner and with greater precision, flexibility and control.
Although cystectomy is usually performed to treat invasive bladder cancer, it can also be performed when the tumor is not muscle infiltrating (or invasive) but fails other treatments.
Bladder preservation by trimodal or multimodal therapy
In very selected patients with infiltrating cancer, with tumors with favorable conditions or which are not suitable for cystectomy, it is possible to preserve the bladder by subjecting the patient to a combined treatment of transurethral resection (TUR bladder resection), chemotherapy and radiotherapy. This is what we call a trimodal treatment and, before carrying it out, a very exhaustive evaluation of the characteristics of the tumor and of the patient must be carried out within a multidisciplinary committee.
Systemic chemotherapy
This is the administration of chemotherapy drugs orally or intravenously. The drugs enter the bloodstream and circulate throughout the body attacking cancer cells distant from the main tumor, i.e. those that have already spread outside the bladder. This is called systemic chemotherapy.
Many of the same drugs used in intravesical chemotherapy are also administered in systemic chemotherapy. The most commonly used are cisplatin; gemcitabine; carboplatin; MVAC, which combines methotrexate, vinblastine, doxorubicin and cisplatin.
It can also be applied after cystectomy in patients with tumor involvement of the perivesical fat or neighboring organs, lymph node involvement, or in patients who already have metastases at the time of diagnosis and who have not undergone surgery. Immunotherapy, i.e. the use of drugs that help the immune system to recognize and destroy cancer cells, is used as a second line of treatment once the disease progresses despite chemotherapy, although there is increasing evidence to support its early use.
Sometimes this chemotherapy is administered as a first step, prior to surgery, to reduce the size of the tumor in patients without lymph node or visceral metastases, which is called neoadjuvant therapy.
Chemotherapy may also be administered after the tumor is removed in order to destroy any cancer cells that may have remained after surgery, called adjuvant therapy.
The side effects of chemotherapy depend on the person and the dose used, but may manifest themselves in the form of fatigue, risk of infection, nausea and vomiting, hair loss, loss of appetite and diarrhea. These side effects usually disappear after the end of treatment.
Radiotherapy:
Radiation therapy uses intensity-modulated rays as part of multimodality treatment to destroy cancer cells that were missed during surgery or as a palliative treatment for incoercible hematuria (bleeding that cannot be contained).
The combination of radiotherapy and chemotherapy after transurethral bladder surgery can sometimes eradicate the cancer without the need for cystectomy.
They ask us in the Consultation
Does a urine culture detect cancer?
No, a urine culture does not detect cancer, as its purpose is to identify urinary tract infections through the presence of bacteria. However, other urine tests, such as a urinalysis or urine cytology, may suggest the presence of cancer by detecting blood or abnormal cells in the urine. If there is suspicion of cancer in the urinary system, additional studies such as biomarker tests, ultrasound, CT scans or biopsies are required to confirm the diagnosis. If you detect blood in the urine with no apparent cause, it is essential to see a physician for further evaluation.
When is it advisable to remove the bladder?
In general, when the tumors are muscle-invasive and have not moved, but are located in the bladder, the bladder must be removed and the urine diverted with a bag to the skin. In very selected patients and with specific characteristics of the tumor, different neobladder techniques can be used.
Is bladder cancer curable?
You have to live with it. It is true that it can be operated, but in the future it can reappear and therefore it is necessary to undergo check-ups to stop it in time. The key is to keep it under control.
What is the prognosis of metastatic bladder cancer?
Most patients do not reach two years. Now there are new treatments with immunotherapies that are achieving longer survivals.
Team of the Bladder Cancer unit
Newsof ROC Clinic in Bladder Cancer
Research
Ureteral metastasis of a prostatic adenocarcinoma
Technology
Radical cystectomy by Da Vinci robotic surgery for maximum precision and minimum aggressiveness.
Training
Training on the controversies in non-muscle invasive bladder and upper urinary tract tumors by Dr. Felix Guerrero Ramos at the AEU.


 +34 912 627 104
+34 912 627 104 Contact
Contact









